Full Body
Skin Exams
Skin cancer is the most common cancer in the United States — and the most survivable when caught early. A full body skin examination by a board-certified FAAD dermatologist, performed annually, is the most effective available tool for detecting basal cell carcinoma, squamous cell carcinoma, and melanoma before they progress. At Couture Dermatology and Laser, every skin exam is conducted with dermoscopy — a magnification technique that improves diagnostic accuracy for melanoma by approximately 30% over the naked eye — and biopsies are performed in-office on the same visit when clinically indicated.
skin cancer by age 70
with dermoscopy
dermatologist
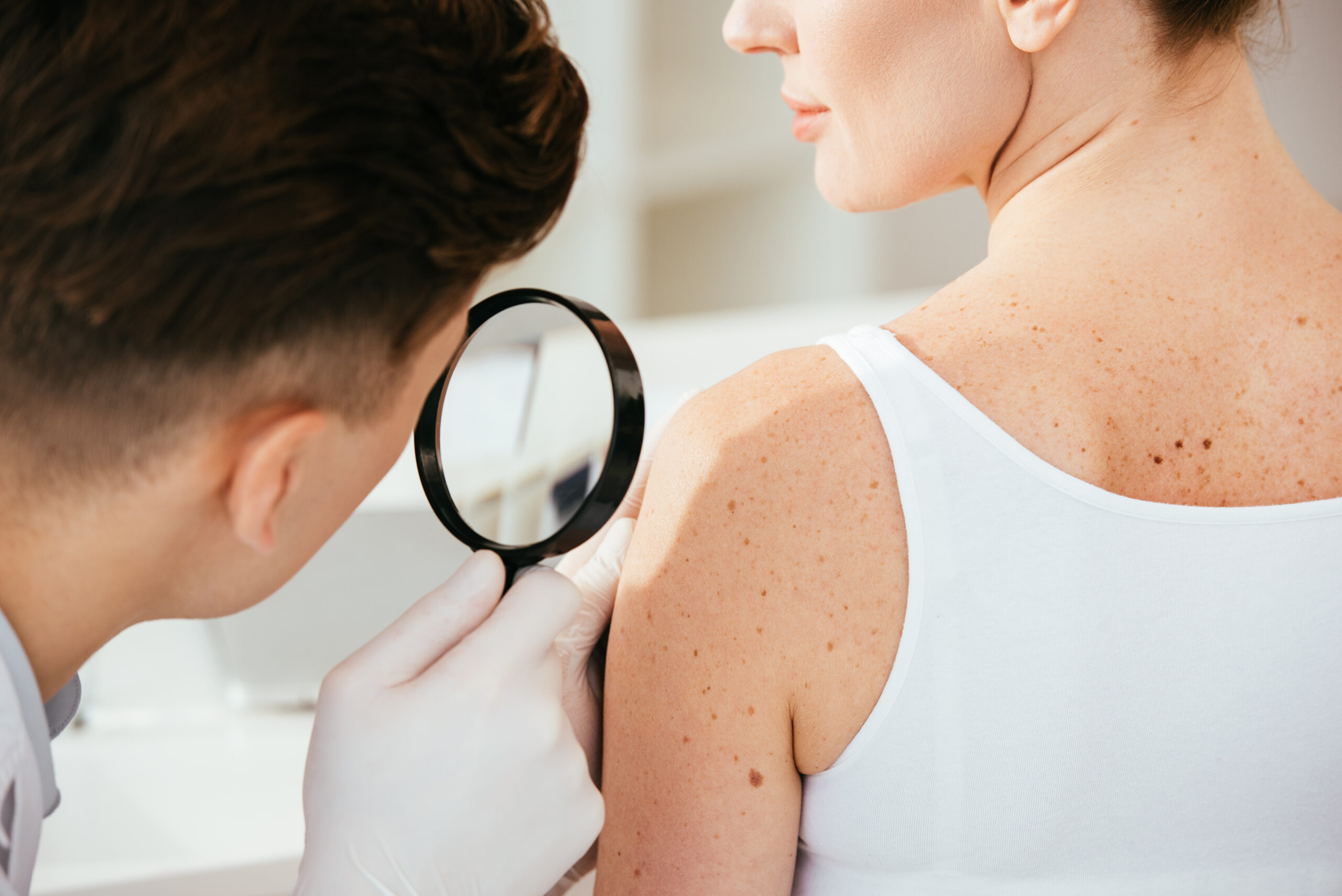
"The best outcome in skin cancer is the one that never requires treatment beyond a simple in-office biopsy — because it was caught early."
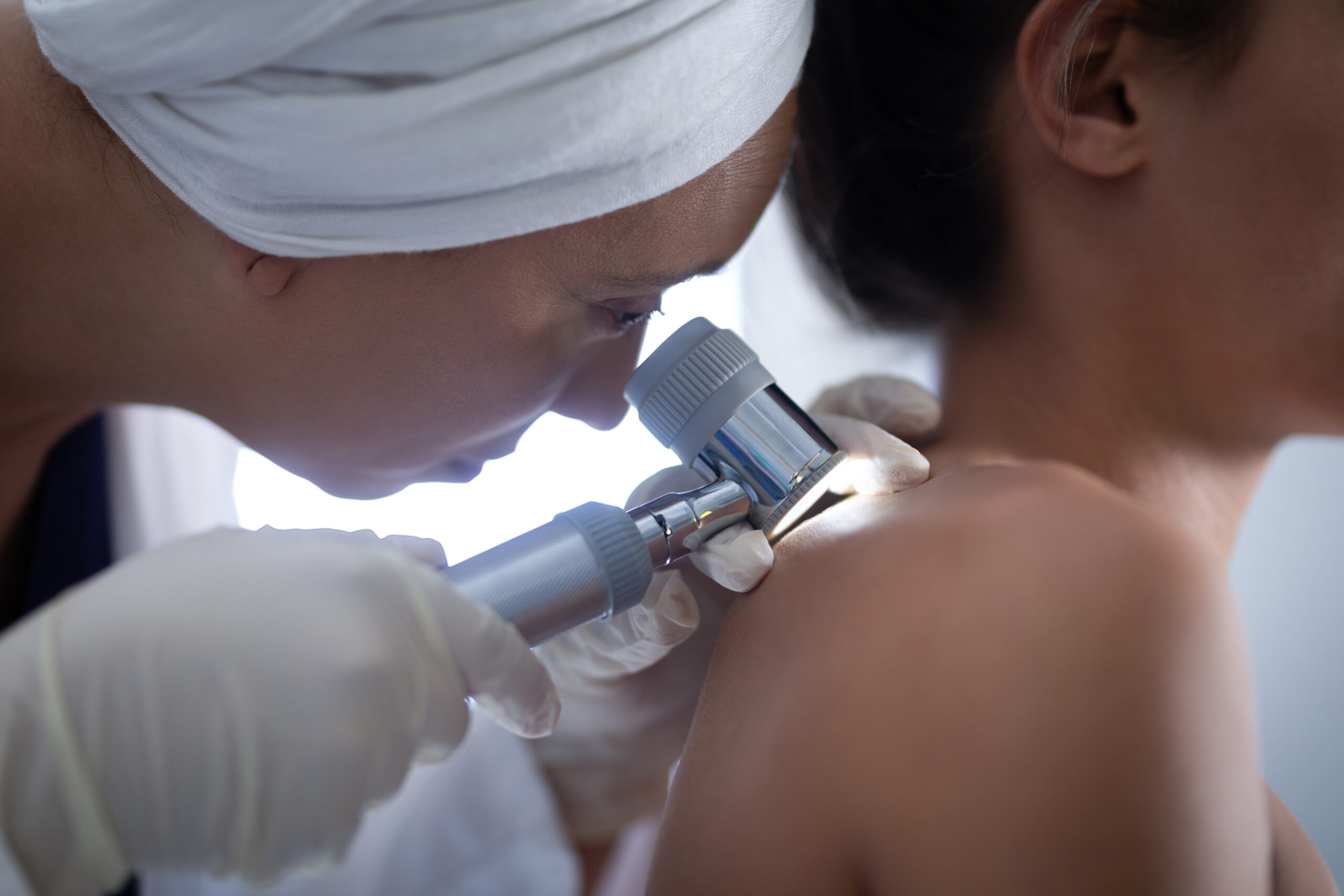
A Systematic Head-to-Toe
Examination of Every Skin Surface.
A total body skin examination (TBSE) is a systematic, methodical examination of every skin surface — scalp, face, ears, neck, chest, abdomen, back, arms, hands, groin, genitals, legs, feet, and soles — conducted by a board-certified dermatologist. It is not a cursory visual sweep; it is a structured clinical assessment in which each anatomical area is examined in sequence using both naked-eye inspection and dermoscopy.
Dermoscopy uses a handheld lens that magnifies the skin surface ×10 to ×40 with polarised light, eliminating surface reflection and revealing subsurface pigment architecture, vascular patterns, and structural features invisible to the naked eye. In trained hands, dermoscopy improves melanoma diagnostic sensitivity by approximately 30% over the unaided eye and reduces unnecessary biopsies of benign lesions.
The exam concludes with a clear communication of every finding — what was seen, what was evaluated dermoscopically, what was considered benign, and what requires either monitoring, biopsy, or further assessment. Where a biopsy is indicated, it is performed at the same appointment.
The Three Primary Skin Cancers
and What They Look Like.
Skin cancer is not a single disease. Basal cell carcinoma, squamous cell carcinoma, and melanoma have distinct appearances, locations, and risk profiles — and different urgency for treatment.
Basal Cell Carcinoma
BCC is the most common human cancer — approximately 80% of all skin cancers. It grows slowly, almost never metastasises, but causes progressive local tissue destruction if untreated. Classic presentation is a pearly or translucent papule with telangiectatic vessels on sun-exposed skin.
Squamous Cell Carcinoma
SCC arises from keratinocytes and accounts for approximately 20% of skin cancers. Unlike BCC, SCC has meaningful metastatic potential (~4%), rising substantially in high-risk variants. Appears as a firm, scaly, keratotic plaque or nodule on sun-damaged skin.
Melanoma
Melanoma arises from melanocytes and is the most dangerous form of skin cancer. Although only ~1% of skin cancers, it causes the majority of skin cancer deaths. Early detection is critical: the 5-year survival for thin melanoma exceeds 95%; advanced melanoma carries substantially worse prognosis.
The ABCDE Rule for
Melanoma Warning Signs
Monthly self-examination between annual professional skin exams is recommended. These are the visual warning signs of melanoma to look for.
One half of the lesion does not mirror the other. A benign mole would produce two roughly equal halves.
Irregular, ragged, notched, or blurred edges — rather than the smooth, well-defined border of a benign mole.
Variation in colour within a single lesion — multiple shades of brown, black, red, white, or blue.
Greater than 6mm — approximately the diameter of a pencil eraser. Melanomas can be diagnosed smaller if other features are present.
Any change in size, shape, colour, or new symptoms — bleeding, itching, crusting. Arguably the most important criterion.
When a Biopsy Is Needed.
Same Day, In-Office.
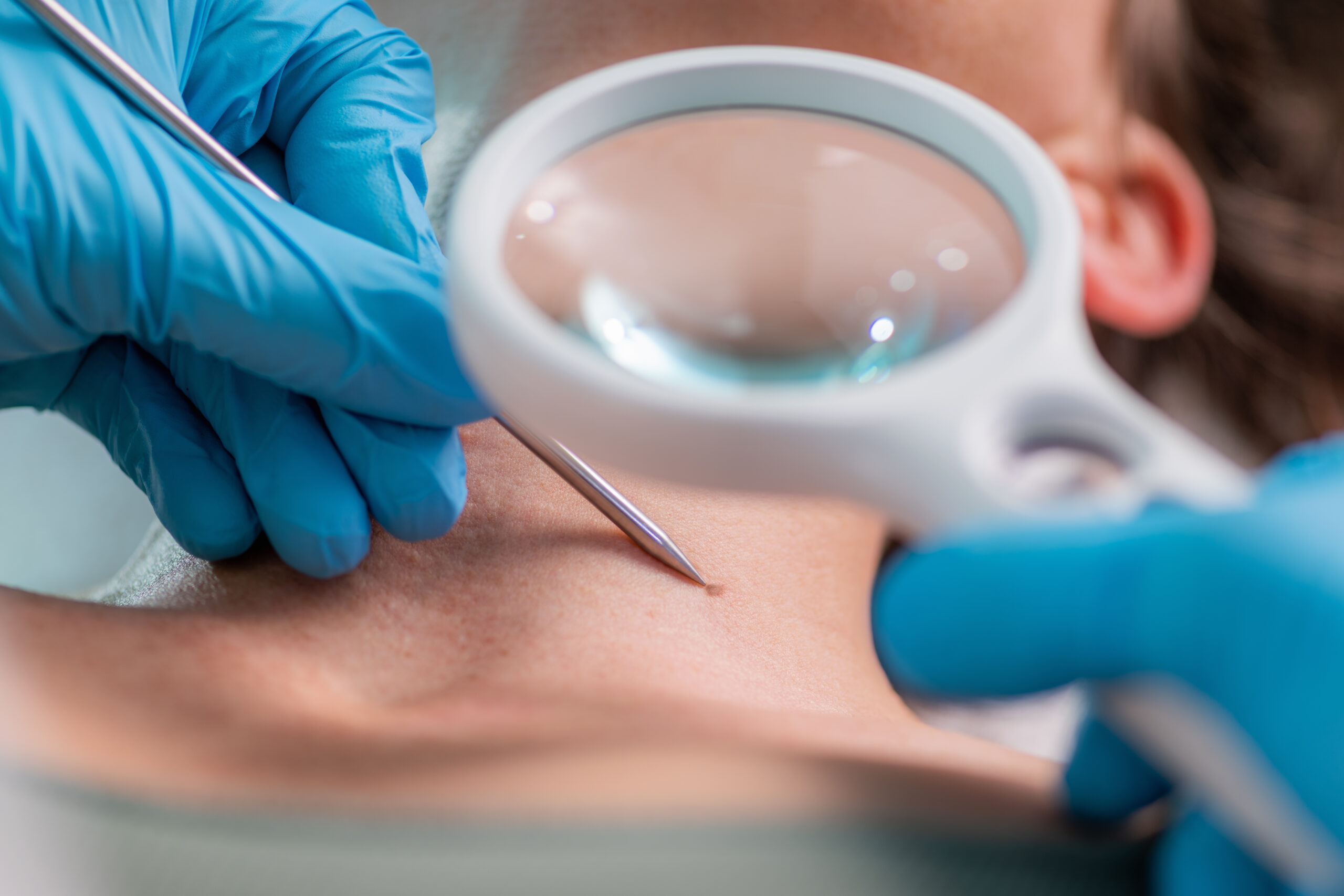
When a lesion warrants tissue diagnosis, a biopsy is performed at the same appointment under local anaesthetic. The type depends on the suspected diagnosis and lesion morphology.
A shave biopsy removes the superficial layer. An excisional biopsy removes the entire lesion with a narrow margin — preferred for suspected melanoma. A punch biopsy uses a circular tool for full-thickness sampling. All specimens are processed by a dermatopathologist.
Results are available within 5–7 business days. Your dermatologist contacts you directly to communicate the result. Where the biopsy confirms skin cancer, the next step is explained clearly.
From Booking to
Results
History & Risk Assessment
Review of skin cancer risk factors: personal and family history, sun exposure, sunburn history, immune status, and any lesions of concern.
5–10 minutesFull Body Examination
Systematic examination of every skin surface: scalp, face, ears, neck, chest, abdomen, back, arms, hands, genital area, legs, feet, and soles. Dermoscopy applied to all moles.
20–30 minutesDermoscopy & Decision
Every mole assessed dermoscopically. Lesions classified as benign, requiring monitoring (with baseline photography), or requiring biopsy. Decisions explained in full.
Explained in fullBiopsy If Indicated
Performed same-day under local anaesthetic. Results in 5–7 business days. Your dermatologist calls with the result and discusses next steps.
Same-day · Results 5–7 daysRisk Factors That Elevate
Your Skin Cancer Risk
Annual screening is recommended for all adults. These factors indicate elevated risk — and typically justify more frequent monitoring.
Prior Skin Cancer or Atypical Moles
The single strongest predictor of future skin cancer. Up to 50% of patients treated for one BCC will develop another within 5 years.
Fair Skin, Light Eyes & Red/Blonde Hair
Fitzpatrick skin types I and II have the highest UV damage accumulation per unit of sun exposure.
Significant Lifetime UV Exposure
Tanning bed use before age 35 increases melanoma risk by approximately 75%. Cumulative UV is the primary determinant of BCC and SCC risk.
Family History of Melanoma
A first-degree relative with melanoma approximately doubles an individual's melanoma risk.
Organ Transplant Recipients
SCC risk is increased approximately 65–250-fold due to long-term immunosuppression. Screening every 3–6 months is recommended.
History of Blistering Sunburns
Five or more blistering sunburns between ages 15–20 are associated with ~80% increase in lifetime melanoma risk.
Board-Certified FAAD
Every skin exam and biopsy performed personally by a board-certified Fellow of the American Academy of Dermatology
Dermoscopy at Every Exam
Improving melanoma diagnostic accuracy by approximately 30% over the unaided eye
Biopsy Same Day
Shave, punch, and excisional biopsies performed in-office at the same visit when clinically indicated
Beverly Hills Location
Couture Dermatology and Laser · Beverly Hills, CA 90212 · (310) 444-0946
The Short Answer:
Every Adult. Annually.
What to do between annual skin exams
Monthly self-examination is recommended. Know your moles: most people have 10–40 moles; you should know roughly where they are so that a new lesion or change is detectable.
Daily SPF 30+ broad-spectrum sunscreen on all sun-exposed skin is the most evidence-supported preventive intervention for skin cancer.
The Best Outcome Is a
Skin Cancer That Never Progresses.
A thin melanoma caught during a routine annual skin exam requires a wide local excision and carries greater than 95% five-year survival. The annual skin exam is not a precaution — it is the most cost-effective intervention in dermatological oncology.
Beverly Hills, CA 90212 · Mon – Fri · 8AM – 5PM · Sat · By Appointment Only
"I had never had a proper skin exam before moving to Beverly Hills. Dr. Chinonso found a mole on my back that turned out to be an early melanoma — caught at the thinnest stage. The biopsy was done the same day. I cannot overstate how important that one appointment was."
Jonathan M.
Verified Patient · Beverly Hills
Results That Speak for Themselves
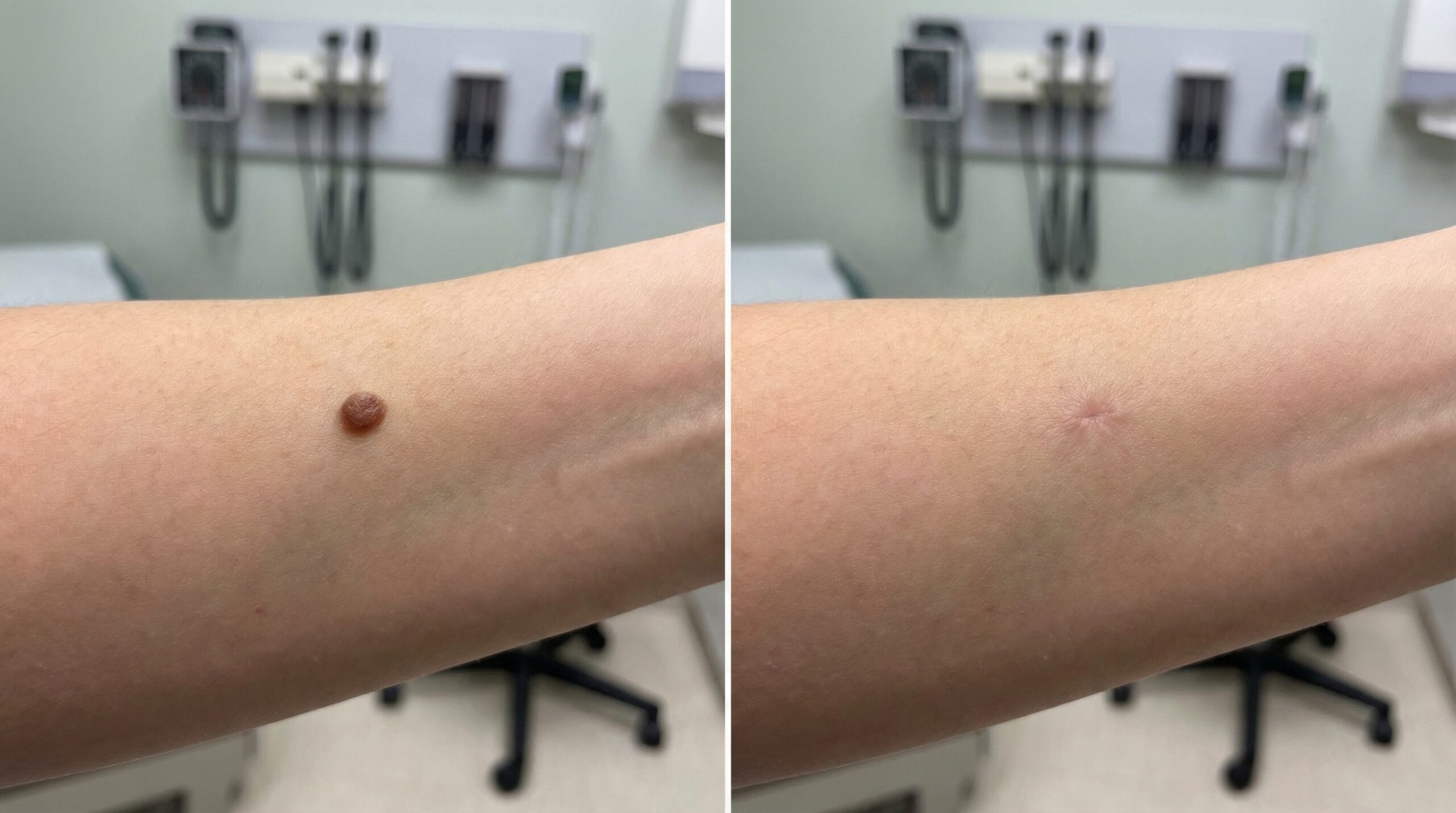
Individual results vary. Images represent outcomes achievable through a personalised treatment programme at Couture Dermatology and Laser.
Frequently
Asked Questions
Direct answers to the most common questions about skin cancer screening, what the exam involves, and when to be concerned about a mole or lesion.
Annual full body skin exams are recommended for all adults. Patients with elevated risk factors require more frequent monitoring: every 3–6 months for prior melanoma; every 6–12 months for prior skin cancer, atypical moles, or family history of melanoma; and every 3–6 months for organ transplant recipients.
Dermoscopy uses a handheld lens with polarised light to magnify the skin ×10–40, revealing subsurface structures invisible to the naked eye. In trained hands, it improves melanoma diagnostic accuracy by approximately 30%. At Couture Dermatology and Laser, dermoscopy is used at every skin examination.
A biopsy is performed at the same appointment under local anaesthetic. Shave, excisional, and punch biopsies are all available in-office. Results are available in 5–7 business days. Your dermatologist contacts you directly with the result and discusses next steps.
Asymmetry, Border irregularity, Colour variation, Diameter greater than 6mm, and Evolution (any change). Any lesion meeting one or more criteria warrants evaluation. Nodular and amelanotic melanoma may not follow the classic pattern.
Basal cell carcinoma (most common, rarely metastasises), squamous cell carcinoma (~4% metastatic risk), and melanoma (highest metastatic potential, prognosis depends on depth at diagnosis). Early detection of all three is the purpose of the annual skin exam.
Prior skin cancer, fair skin and light eyes, significant UV exposure including tanning beds, family history of melanoma, organ transplant recipients on immunosuppression, and history of blistering sunburns in youth. Southern California's year-round UV elevates baseline risk across all populations.

