Psoriasis
Treatment
Psoriasis begins in the immune system, not on the skin surface. The rapid cell turnover that produces its characteristic plaques is fueled by a specific cytokine pathway. At Couture Dermatology and Laser, psoriasis management is calibrated to your subtype, severity, and life — from prescription topical therapy through to biologic agents that achieve complete skin clearance in the majority of patients.
biologic patients
arthritis
Dermatologist
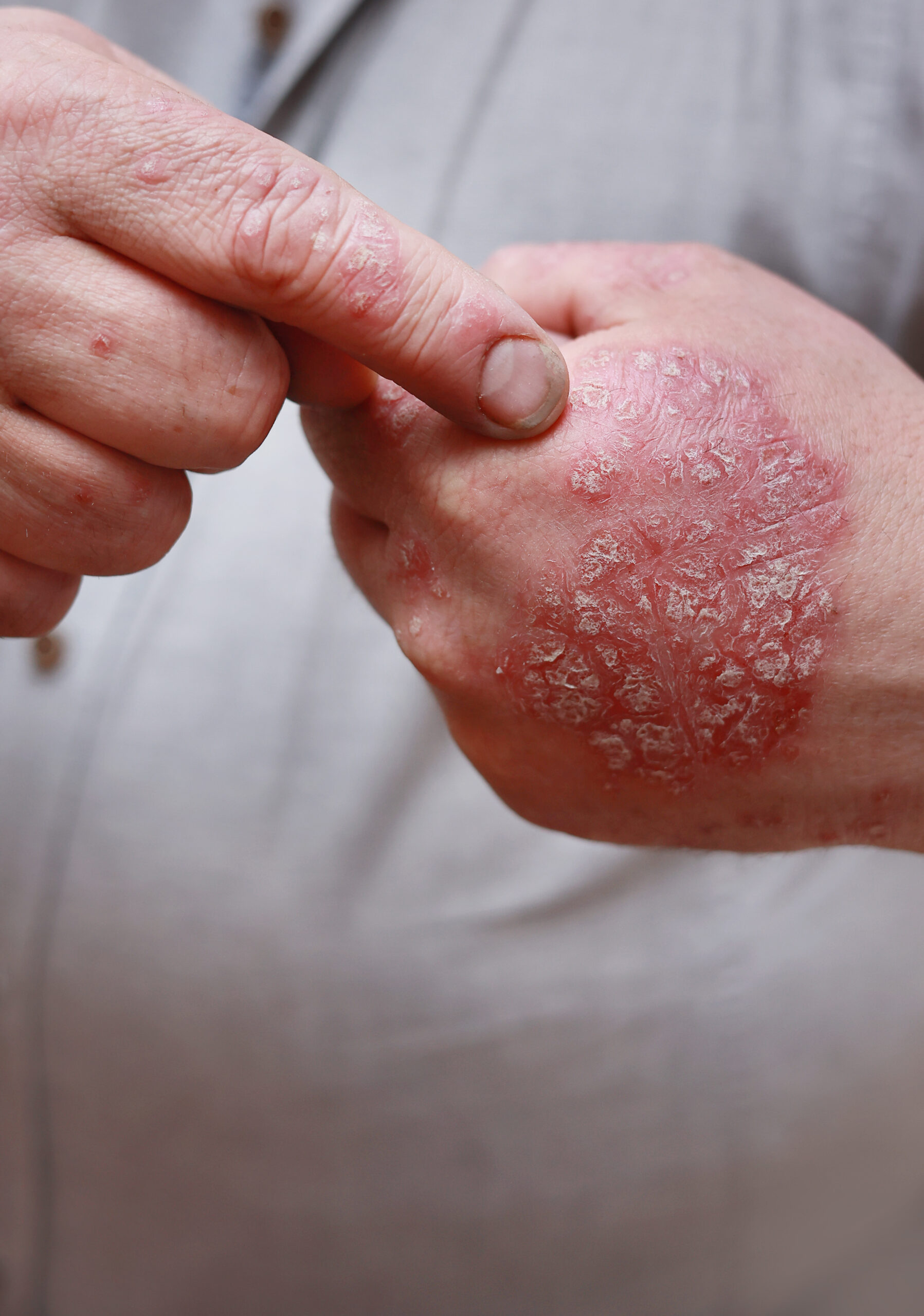
"Modern biologic therapy achieves complete or near-complete skin clearance in the majority of moderate-to-severe patients."
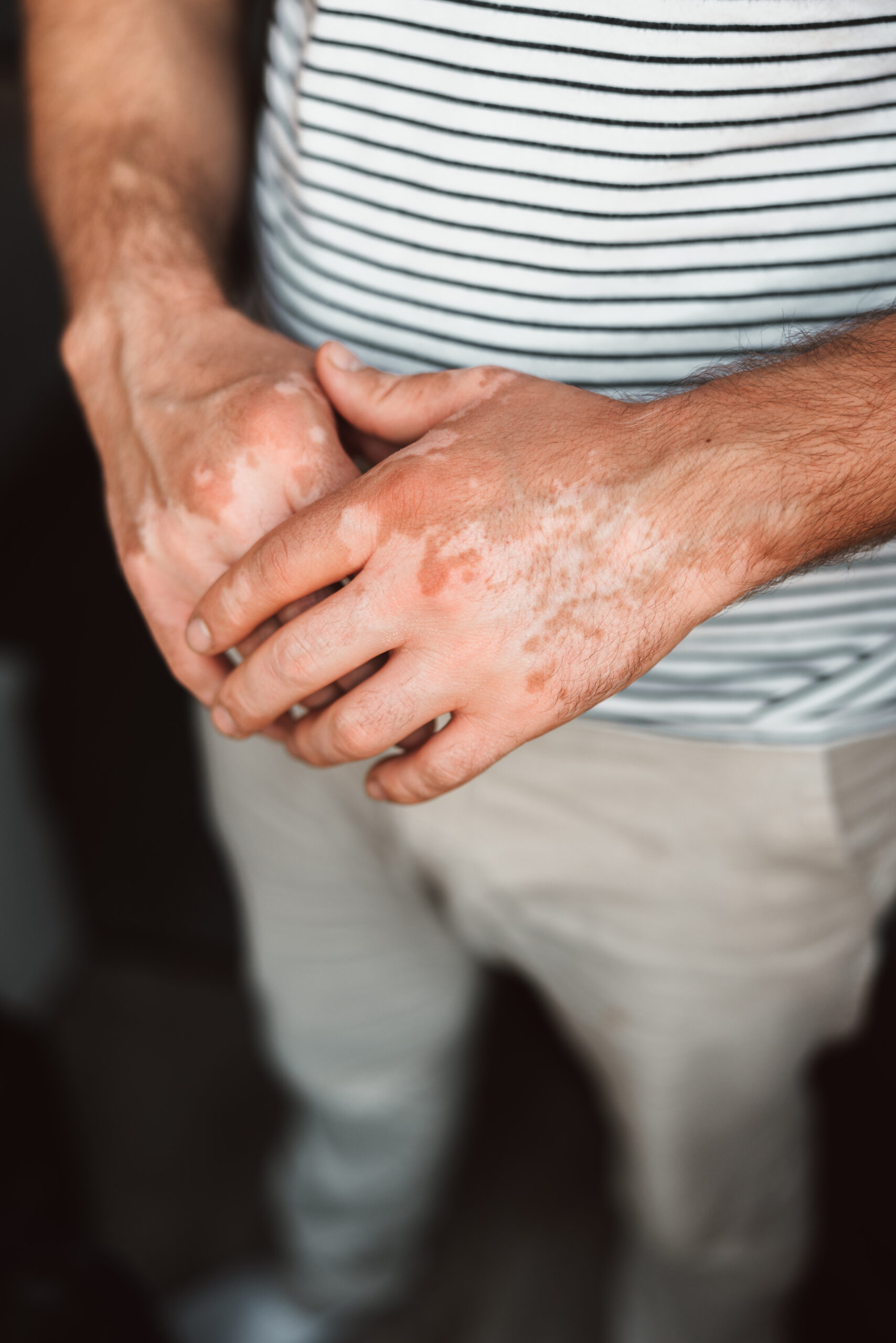
An Immune Condition.
Not a Surface Problem.
Psoriasis begins in the immune system. Activated T-cells—incorrectly recognising skin proteins as foreign—release inflammatory cytokines that signal skin cells to proliferate at dramatically accelerated speed. This cycle compresses from 28 days down to 3–5 days, producing the characteristic raised, silvery-scaled plaques on the surface.
The IL-23/IL-17 axis is the primary driver of this immune dysregulation. This is why modern therapies—IL-23 and IL-17 inhibitors—achieve plaque clearance rates that earlier treatments could not approach. While psoriasis has a strong genetic component, environmental triggers like stress or infection activate it.
Psoriasis is systemic. Managing it comprehensively means screening for associated psoriatic arthritis, cardiovascular risk, and inflammatory bowel disease, coordinating care where indicated.
Six Subtypes.
Each Behaves Differently.
Subtype determines distribution, severity, and treatment selection. Most patients have predominantly one subtype, though overlap is common.
Plaque Psoriasis
80–90% of cases. Raised, erythematous plaques covered by a silver-white scale. Classic sites include elbows, knees, scalp, and lower back.
Guttate Psoriasis
An acute eruption of small, drop-shaped scaly papules, classically triggered by a streptococcal throat infection in younger patients.
Pustular Psoriasis
Characterised by sterile pustules on an erythematous base. Can be localised to palms/soles, or generalized, requiring urgent systemic care.
Nail Psoriasis
Pitting, onycholysis, and subungual hyperkeratosis. A strong clinical predictor for the development of psoriatic arthritis.
Erythrodermic Psoriasis
A rare dermatological emergency involving >90% body surface area with intense redness and exfoliation. Requires immediate intervention.
Inverse Psoriasis
Smooth, red, inflamed lesions found exclusively in body folds (axillae, groin, under breasts), often lacking typical silver scale due to moisture.
From Consultation
to Sustained Clearance
Psoriasis management follows a well-defined treatment ladder calibrated to your specific severity and disease impact.
Severity Assessment
Your dermatologist assesses subtype, PASI score, body surface area, and quality-of-life impact. Special sites (scalp, nails, genitals) elevate functional severity.
Complete at first visitComorbidity Screen
Psoriatic arthritis is screened systematically. Cardiovascular risk and inflammatory bowel disease history are noted, as they directly influence biologic selection.
Before biologic prescribingTreatment Selection
Treatment is selected based on severity tier and history. Mild disease uses optimized topicals; moderate-to-severe disease opens the discussion to targeted biologic therapy.
Informed patient decisionMonitoring
For patients on biologics, response is assessed at 12–16 weeks. Patients achieving PASI 90 or better are maintained; others are reviewed for dose optimization or switching.
12–16 week assessmentThe Evidence
Behind the Options
Psoriasis treatment has a well-defined hierarchy of efficacy, from topical agents through to the most advanced biologic therapies available.
Mild Disease · First-Line
Topical Therapies
The cornerstone of mild management. Prescription corticosteroids suppress local inflammation, while vitamin D analogues normalise cell turnover. Their combination in a single formulation is highly evidence-supported. Effective for limited disease but practically inadequate for large surface areas.
Moderate Disease · Second-Line
Narrowband UVB Phototherapy
Delivered at 311–313nm, NB-UVB suppresses the T-cell driven inflammatory response, producing plaque clearance across the whole body. A typical course is 20–30 sessions, achieving PASI 75 in ~70% of patients. Safe in pregnancy and an excellent bridge to biologics.
Moderate-Severe · Targeted
IL-17 Inhibitors
The fastest class of biologics for plaque psoriasis (secukinumab, ixekizumab, bimekizumab). By blocking the primary downstream cytokine driving hyperproliferation, they achieve PASI 90 in 70–80% of patients at 12–16 weeks. Also highly effective for concurrent psoriatic arthritis.
Moderate-Severe · Durable
IL-23 Inhibitors
Acting upstream (guselkumab, risankizumab), they block the survival of Th17 cells. This produces more durable responses with less frequent dosing (every 8–12 weeks). They have an excellent safety profile, particularly for patients with coexisting inflammatory bowel disease.
A Systemic
Inflammatory Condition.
Psoriatic Arthritis
Affects ~30% of patients. Often presenting years after the skin condition, it can be destructive without early treatment. Nail psoriasis is the strongest predictor of joint involvement.
Cardiovascular Disease
Moderate-to-severe psoriasis is an independent cardiovascular risk factor. Chronic systemic inflammation drives atherosclerosis. Effective biologic control is associated with reduced cardiovascular event rates.
Metabolic Syndrome
Psoriasis patients have elevated rates of obesity, hypertension, and insulin resistance. This bidirectional relationship means metabolic syndrome worsens psoriasis severity, while weight loss improves biologic response.
Inflammatory Bowel Disease
Crohn's and ulcerative colitis occur at elevated rates due to shared genetic susceptibility loci. IBD history is critical to biologic selection, as IL-17 inhibitors are contraindicated in active Crohn's.
"Managing psoriasis comprehensively means managing it as the systemic inflammatory condition it is."— Couture Dermatology and Laser

Arthritis
Board-Certified FAAD
Every psoriasis programme assessed, prescribed, and monitored personally by a Harvard-trained dermatologist
Biologic Prescribing
IL-17 and IL-23 biologics prescribed and monitored entirely in-practice — no external referral required
Arthritis Screening
Systematic joint screening at every visit — rheumatology referral coordinated where PsA is confirmed
Beverly Hills Location
Couture Dermatology and Laser · Beverly Hills, CA 90212 · (310) 444-0946
When to See a
Dermatologist
- Adults or children with an uncertain diagnosis being managed as eczema without response.
- Patients with moderate-to-severe plaque psoriasis who want to discuss biologic therapy options.
- Anyone with psoriasis and joint symptoms — pain, swelling, morning stiffness, or swollen digits.
- Patients on older systemic therapies (methotrexate, ciclosporin) not achieving satisfactory clearance.
- Those whose psoriasis significantly affects quality of life — sleep, clothing, or self-confidence — regardless of BSA.
Honest Expectations
Psoriasis cannot be permanently cured — the underlying genetic predisposition does not resolve. What does change, dramatically, is the level of active disease. For patients with moderate-to-severe disease on appropriate biologic therapy, complete or near-complete skin clearance is a realistic and frequently achieved outcome.
The most important factor is matching treatment tier to disease severity. We assess your severity honestly and discuss the full range of options at consultation.
Conditions Treated
Alongside Psoriasis
Inflammatory skin conditions often overlap. We manage the full spectrum of autoimmune dermatological concerns.
Eczema (Atopic Dermatitis)
Chronic inflammatory skin condition driven by barrier dysfunction and Th2 immune dysregulation — managed with dupilumab biologic therapy.
Explore eczema →Skin Rashes & Dermatitis
Inflammatory rashes — contact dermatitis, drug reactions, and urticaria — diagnosed clinically and with patch testing.
Explore skin rashes →Alopecia & Hair Loss
Scarring alopecias and inflammatory scalp conditions that can sometimes mimic or coexist with scalp psoriasis.
Explore hair loss →Rosacea
Chronic facial erythema and inflammatory papulopustular disease managed with vascular laser and systemic anti-inflammatory therapy.
Explore rosacea →Psoriasis That No Longer
Defines Your Skin.
Modern biologic therapy has transformed the outlook for moderate-to-severe psoriasis. PASI 90 — skin that is 90% clear — is now a realistic benchmark. If your current management is not producing this level of clearance, we start with an honest assessment of your options.
Sat · By Appointment Only
"I had been managing my psoriasis poorly for years. Dr. Chinonso reviewed my entire history and changed my treatment approach completely. The plaques have cleared more than they ever have with previous dermatologists. She genuinely cares about long-term management, not quick fixes."
Rebecca O.
Verified Patient · Beverly Hills
Results That Speak for Themselves
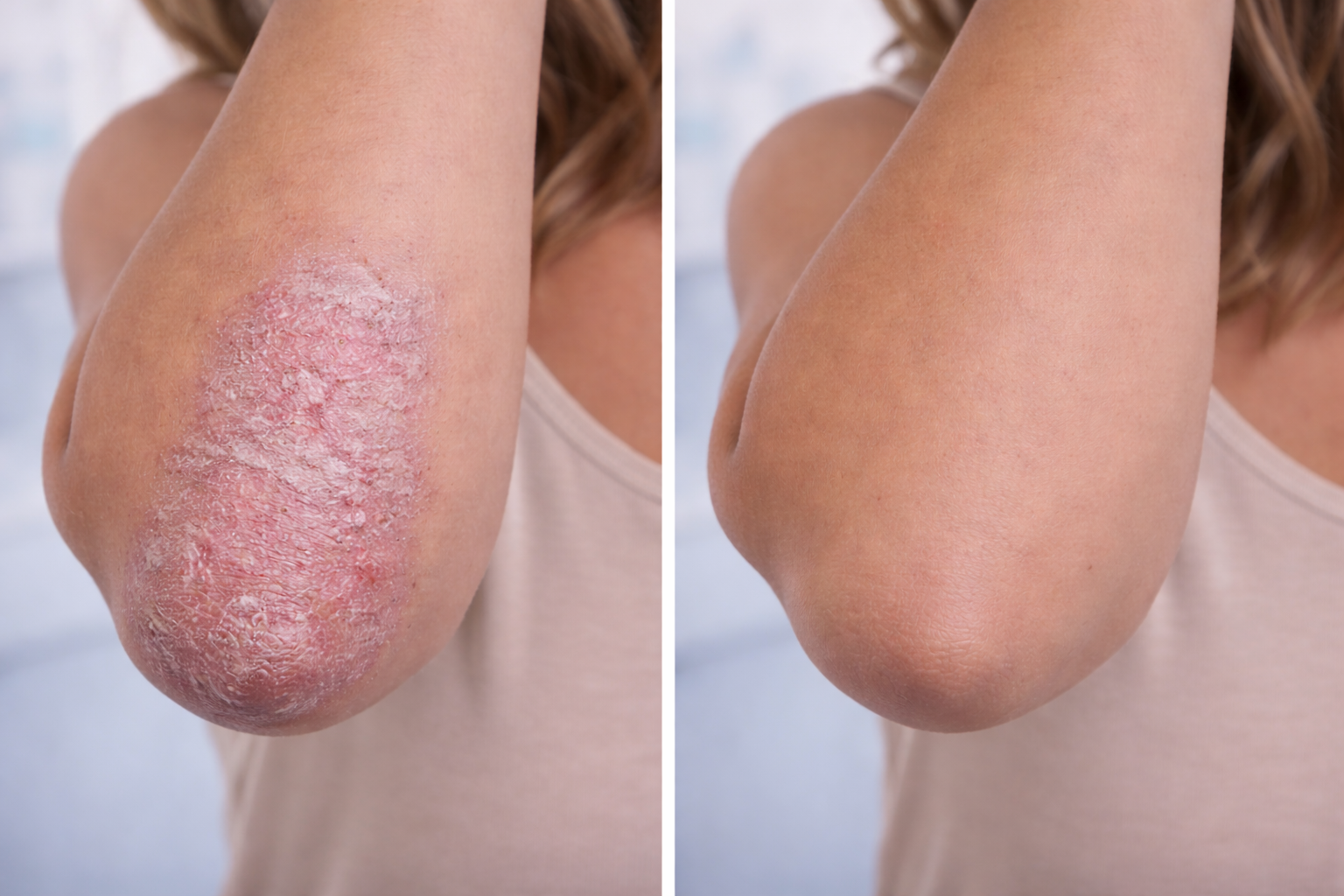
Individual results vary. Images represent outcomes achievable through a personalised treatment programme at Couture Dermatology and Laser.
Frequently
Asked Questions
Direct answers to the questions psoriasis patients most commonly bring to consultation — on the condition's cause, joint disease associations, and what modern treatment can achieve.
Psoriasis is caused by immune dysregulation — an overactive T-cell response driven by IL-17 and IL-23 signalling that stimulates keratinocytes to proliferate. In healthy skin, epidermal cells take 28 days to mature; in psoriasis, this is compressed to 3–5 days, producing scale. It has a strong genetic component, triggered by stress, infection, or medications.
No. Psoriasis is not contagious — it cannot be transmitted through skin contact or sharing clothing. It is an autoimmune condition driven by the patient's own immune system; the plaques contain no infectious agent.
Biologics are injectable proteins that target specific cytokines driving psoriasis inflammation. IL-17 and IL-23 inhibitors achieve PASI 90 (90% reduction in plaque severity) in the majority of patients with moderate-to-severe disease. They are administered every 2–12 weeks. Suitability depends on disease severity and medical history.
Psoriatic arthritis (PsA) is an inflammatory joint condition occurring in ~30% of psoriasis patients. It presents as painful, swollen joints with morning stiffness. Nail psoriasis is a strong predictor. It requires rheumatology involvement alongside dermatological skin management. Several biologics treat both skin and joints.
Triggers include psychological stress, streptococcal throat infection (triggering guttate psoriasis), certain medications (lithium, beta-blockers), skin injury (Koebner phenomenon), smoking, and alcohol excess. Identifying and managing individual triggers is discussed as part of every management programme.
Psoriasis cannot be permanently cured, but it can be managed to a state of minimal or no visible disease. Modern biologic therapy produces complete or near-complete skin clearance in the majority of moderate-to-severe patients. The goal is skin that does not limit daily life or confidence.
Related Treatments
Psoriasis Treatment
in Beverly Hills, CA
Couture Dermatology offers expert care for Psoriasis in Beverly Hills, CA, providing personalized treatment plans to help manage this chronic skin condition. Our experienced dermatologists use advanced therapies to reduce symptoms and improve quality of life. We are committed to supporting you with compassionate care and the latest medical solutions.

Understanding Psoriasis
Common Signs and Symptoms of Psoriasis
Red, Raised Skin Patches
Silvery Scales Formation
Persistent Itching and Discomfort
Cracked or Bleeding Skin
Nail Changes
Primary Causes and Triggers of Psoriasis
Effective Psoriasis Treatment Options
- Topical corticosteroids help reduce inflammation and relieve itching.
- Phototherapy uses controlled ultraviolet light to slow skin cell growth.
- Systemic medications can treat moderate to severe cases from within the body.
- Biologic therapies target specific immune responses causing psoriasis.
- Moisturizers and emollients soothe dryness and help heal the skin barrier.
- Lifestyle modifications such as stress management can minimize flare-ups.
Who Is a Good Candidate
- Individuals experiencing persistent red, scaly skin patches are ideal candidates for psoriasis treatment.
- People whose symptoms interfere with daily comfort or confidence may benefit from treatment.
- Candidates include patients who have not responded to over-the-counter therapies.
- Those with psoriasis-related nail changes or joint pain should consider advanced care.
Check Your Insurance Coverage
Psoriasis Treatment Benefits
Symptom Relief and Comfort
Improved Skin Appearance
Enhanced Quality of Life
Long-Term Health Protection
Dr. Chinonso Kagha
Abisogun, MD, FAAD
Why Choose Couture Dermatology for Psoriasis Treatment
At Couture Dermatology, our board-certified dermatologists offer advanced, individualized care for psoriasis. We utilize the latest therapies and a compassionate approach to help you achieve clearer skin and better symptom control. Our Beverly Hills, CA, clinic is dedicated to supporting your journey with expert guidance and a commitment to lasting results.
Check Your Insurance Coverage
Testimonials

- Rosie D.
Healthy Skin.
Beautiful
Complexion.
A More Confident You.

