Rosacea
Treatment
Rosacea is a chronic inflammatory skin condition — not simply sensitive skin or occasional redness. At Couture Dermatology and Laser, your board-certified FAAD dermatologist classifies your specific subtype and identifies your triggers before selecting any treatment — because the right approach depends entirely on which form of rosacea is present.
vascular rosacea
redness resolution
dermatologist

"Rosacea is managed — not cured. The goal is skin that is no longer visibly dominated by redness."
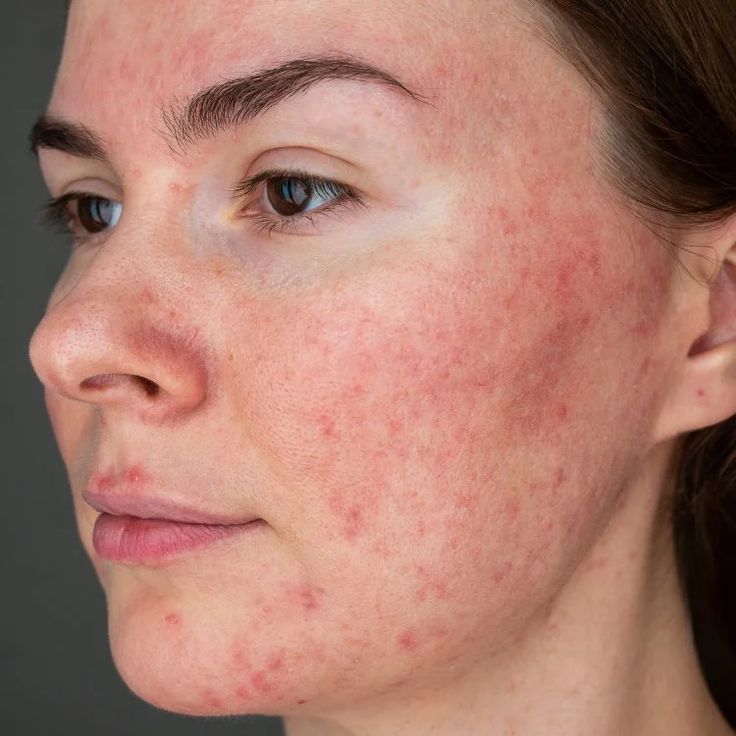
A Chronic Condition.
Correctly Classified.
Rosacea is a chronic inflammatory skin condition affecting the central face. Its most visible feature is persistent facial redness, but it encompasses a spectrum of presentations driven by different mechanisms: vascular hyperreactivity, neurovascular dysregulation, and immune-mediated inflammation.
It is not sensitive skin that needs gentler products. It is not acne — though the papulopustular subtype can resemble it. Without management, it typically progresses over years — flares becoming more frequent, background erythema more persistent, and visible vessels more numerous.
At Couture Dermatology and Laser, management combines clinical treatment of existing vascular and inflammatory disease with practical trigger identification — because laser suppresses active rosacea, but trigger avoidance reduces the frequency of new flares.
Four Subtypes.
Different Approaches.
Rosacea is not a single condition — it is a family of related inflammatory presentations. Treatment selection depends entirely on which subtype is present.
ETR · Vascular Subtype
Erythematotelangiectatic
The most common subtype — characterised by persistent central redness, episodic flushing triggered by heat, alcohol, or UV, and progressively visible telangiectasia (dilated blood vessels). ETR is fundamentally a vascular condition: blood vessels are abnormally reactive, remaining dilated rather than returning to baseline.
PPR · Inflammatory Subtype
Papulopustular Rosacea
Presents with the persistent central erythema of ETR alongside inflammatory papules and pustules — the presentation most commonly mistaken for acne. The critical distinction: PPR does not produce comedones (blackheads). Treating PPR with acne therapies often worsens the condition by damaging the barrier.
Tissue Overgrowth Subtype
Phymatous Rosacea
Involves progressive skin thickening and tissue overgrowth — most commonly rhinophyma (thickening of the nose). The sebaceous glands hypertrophy, and connective tissue proliferates, producing an irregular surface texture. Represents the advanced end of rosacea progression over years without management.
Eye Involvement Subtype
Ocular Rosacea
Affects the eyes in approximately 50% of rosacea patients — often preceding cutaneous disease. Symptoms include chronic redness of the sclera, a gritty sensation, sensitivity to light, and recurrent styes. Frequently underdiagnosed because patients do not associate eye symptoms with their facial skin.
How Your Rosacea Programme
Is Structured
Rosacea management combines clinical treatment of existing disease with a structured approach to trigger reduction — both are required for lasting control.
Assessment
Your FAAD dermatologist classifies your rosacea subtype and evaluates the severity of erythema, telangiectasia, and inflammatory lesions.
Included at every visitTrigger ID
A practical trigger avoidance framework is discussed to reduce your specific flare frequency alongside clinical treatment.
Personalised mapClinical Treatment
Vascular laser or IPL targets dilated vessels. Prescription topical or oral therapies suppress the inflammatory component where indicated.
20–40 minutesMaintenance
After the initial series, ongoing management is required to prevent relapse. Maintenance laser sessions every 6–12 months address new vessels.
6–12 month intervalsThe Right Modality
for Each Component
Rosacea has a vascular component and, in many patients, an inflammatory component. These are treated differently, and most programmes combine both.
ETR · Telangiectasia · Visible Vessels
Vascular Laser (PDL / Nd:YAG)
Pulsed dye laser (PDL) and long-pulsed Nd:YAG deliver selective photothermolysis — targeting oxyhemoglobin in dilated vessels. The thermal energy collapses the vessel wall; the body reabsorbs it over 2–4 weeks. PDL is optimal for fine facial telangiectasia; Nd:YAG penetrates deeper and is the safer choice for darker skin tones.
ETR · Diffuse Erythema
Intense Pulsed Light (IPL)
IPL delivers broad-spectrum light energy that targets haemoglobin. For ETR with diffuse facial erythema — where redness is generalised — IPL treats the entire background in a full-face pass more efficiently than point-by-point laser. IPL also improves skin texture and reduces mild pigmentation.
PPR · Inflammatory Lesions
Prescription Topicals
Prescription agents are the cornerstone of PPR management. Azelaic acid reduces inflammatory lesions. Metronidazole is an established anti-inflammatory. Ivermectin targets the Demodex mite implicated in rosacea pathogenesis. These are prescription-strength formulations; OTC versions lack clinical effect.
Moderate–Severe PPR
Oral Doxycycline
Oral doxycycline at sub-antimicrobial doses is prescribed for moderate-to-severe PPR where topical therapy is insufficient. At this dose, it functions as an anti-inflammatory rather than an antibiotic — suppressing inflammation without the antibiotic selection pressure that drives bacterial resistance.
Skin That Is No Longer
Defined by Redness.
Visible Vessels Cleared
Telangiectasia on the cheeks and nose are targeted by vascular laser. Treated vessels collapse and are reabsorbed over 2–4 weeks — clearing the thread-like red vessels that accumulate progressively without treatment.
Background Erythema Reduced
The persistent diffuse redness that characterises ETR responds progressively to IPL and vascular laser across a series of sessions. Skin tones become more even, and the resting redness is significantly reduced.
Inflammatory Lesions Suppressed
Papulopustular rosacea responds to prescription topical therapy within 4–8 weeks. Inflammatory lesions reduce in frequency and severity, while concurrent oral doxycycline accelerates clearance.
Flare Frequency Reduced
Trigger identification and avoidance, combined with ongoing prescription maintenance therapy, reduces how frequently rosacea flares — not just how severely it presents when it does.
Rosacea That No Longer Dominates
The goal is skin that does not read as rosacea in normal social lighting — a face where persistent redness is no longer the first feature noticed. With consistent management, most patients achieve this.
"Rosacea is managed — not cured. The goal is skin that is no longer visibly dominated by redness in daily life."— Couture Dermatology and Laser

to clear
Board-Certified FAAD
Every rosacea programme designed and delivered personally by a board-certified Fellow of the American Academy of Dermatology
Subtype Classification
ETR, papulopustular, and phymatous subtypes identified individually — rosacea is not treated as a single condition
Trigger Management
Personalised trigger identification built into every programme — clinical treatment and flare avoidance are both required
Beverly Hills Location
Couture Dermatology and Laser · Beverly Hills, CA 90212 · (310) 444-0946
Identifying What
Drives Your Flares
Clinical treatment suppresses existing rosacea. Trigger identification reduces new flare frequency. Managing one without the other produces only partial control.
UV Exposure
The most consistent rosacea trigger. UV radiation activates inflammatory pathways. Daily broad-spectrum mineral SPF 50+ is non-negotiable.
Heat & Temperature
Hot beverages, hot showers, saunas, and heated environments trigger vascular dilation in ETR, increasing flushing frequency.
Alcohol
Red wine is the most potent alcohol trigger — containing histamine and tannins that compound the vascular vasodilatory effect.
Skincare Irritants
Rosacea skin has compromised barrier function. Alcohol-based toners, fragrance, and physical scrubs trigger burning and flares.
Spicy Food & Diet
Spicy food triggers neurogenic flushing via capsaicin. Cinnamaldehyde and high-histamine foods are secondary dietary triggers.
Emotional Stress
Psychological stress triggers catecholamine release that activates the same vascular pathway as physical heat.
Is Rosacea Treatment
Right for You?
- Adults with persistent facial redness, visible thread veins, or episodic flushing that does not resolve with skincare adjustments.
- Patients with inflammatory papules or pustules on the central face — especially where the presentation has been misdiagnosed as acne.
- Those who notice facial redness worsening with identifiable triggers like heat, alcohol, or stress.
- Patients who have previously had rosacea treatment and experienced relapse — wanting a structured maintenance programme.
- Anyone whose rosacea affects their confidence, social approach, or daily experience of their appearance.
Honest expectations for management
Rosacea cannot be permanently cured. Clinical treatment — vascular laser, IPL, prescription topicals — significantly reduces existing disease and slows progression. But rosacea is a chronic inflammatory condition; the underlying vascular hyperreactivity persists. Relapse without maintenance is the rule, not the exception.
The most important factor in long-term rosacea control is consistency — consistent SPF use, trigger management, prescription maintenance therapy, and periodic maintenance laser sessions.
Treatments That Work
Alongside Management
Rosacea management addresses redness and inflammation. These treatments address the accompanying skin quality and pigmentation concerns that often coexist.
Laser Skin Resurfacing
Fractional laser for skin texture and quality — sequenced after rosacea is well-controlled, addressing surface irregularities and pore appearance.
Explore laser resurfacing →Hyperpigmentation
Post-inflammatory pigmentation from rosacea lesions treated alongside the programme with conservative laser calibrated to avoid triggering reactivity.
Explore pigment correction →Age Spot Removal
UV-induced solar lentigines that coexist with rosacea-related erythema — IPL can address both in coordinated sessions when appropriately calibrated.
Explore age spot removal →Microneedling
For skin quality improvement in well-controlled rosacea — collagen induction addressing texture between laser sessions, adapted for barrier fragility.
Explore microneedling →Rosacea That Stays
Under Control.
Rosacea is manageable — but it requires a programme that correctly identifies your subtype, your triggers, and the approach that addresses both the vascular and inflammatory components. At Couture Dermatology and Laser, your board-certified FAAD dermatologist builds that programme at consultation.
Sat · By Appointment Only
"I had lived with persistent redness and flushing for years and had given up on finding a solution. Dr. Chinonso identified my triggers and built a treatment plan that has genuinely transformed my skin. The redness is dramatically reduced and my confidence is back."
Emily F.
Verified Patient · Beverly Hills
Results That Speak for Themselves

Individual results vary. Images represent outcomes achievable through a personalised treatment programme at Couture Dermatology and Laser.
Frequently
Asked Questions
Direct answers to the questions rosacea patients most commonly bring to consultation — on what the condition is, how it is classified, and what management can realistically achieve.
Rosacea is a chronic inflammatory skin condition affecting the central face — primarily the cheeks, nose, forehead, and chin. It is characterised by episodic flushing, persistent erythema, visible telangiectasia, and in some subtypes, inflammatory papules. Rosacea is not acne — it has a different underlying mechanism driven by vascular hyperreactivity and neurovascular dysregulation.
Rosacea is classified into four subtypes: Erythematotelangiectatic rosacea (ETR) presents with persistent redness and visible telangiectasia; Papulopustular rosacea presents with redness alongside inflammatory papules; Phymatous rosacea involves skin thickening (rhinophyma); and Ocular rosacea affects the eyes. Many patients have overlapping subtypes.
Rosacea cannot be permanently cured — it is a chronic condition that requires ongoing management. Treatment significantly reduces flare frequency and severity, clears visible vessels, and suppresses inflammatory lesions. With consistent management, most patients achieve a state where rosacea is not visibly apparent in daily life.
Common rosacea triggers include UV exposure, heat (hot environments or showers), alcohol (particularly red wine), spicy food, emotional stress, and skincare products containing alcohol or fragrance. Identifying your specific trigger profile at consultation is an important part of management.
Most patients with erythematotelangiectatic rosacea see significant improvement after 2–4 vascular laser or IPL sessions spaced 4–6 weeks apart. Visible telangiectasia typically clears in 1–3 sessions. Maintenance sessions every 6–12 months are recommended to address new vessel formation and prevent relapse.
Acne is driven by sebaceous follicle obstruction, bacterial colonisation, and sebum overproduction — producing comedones (blackheads). Rosacea does not produce comedones. Rosacea is driven by vascular hyperreactivity and immune-mediated inflammation. Treating rosacea with acne products is ineffective and often worsening.

